Snapshot
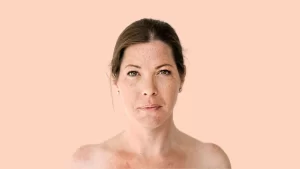
Declining estrogen = weakened urinary tract lining, making women more prone to infections.
Menopausal women face a significantly higher risk of urinary tract infections (UTIs), with postmenopausal women being 2.5-3 times more likely to experience recurrent UTIs compared to their premenopausal counterparts. This increased susceptibility is primarily due to declining estrogen levels, which weaken urinary tract defenses and alter the balance of beneficial bacteria. However, proactive measures such as staying hydrated, considering vaginal estrogen therapy, and using probiotics can substantially reduce UTI occurrences, helping women maintain their quality of life during this transitional phase.
Menopausal UTIs: What’s really happening?
As we move through perimenopause, menopause, and postmenopause, changes in hormone levels can bring some unwelcome surprises—like recurring urinary tract infections (UTIs). Many women wonder, “Why now? I never had so many UTIs before.” The answer lies in estrogen, a key hormone that plays a crucial role in maintaining healthy urinary and vaginal tissue.
When estrogen levels drop, the tissue lining the bladder and urethra becomes thinner, drier, and more fragile. This makes it easier for bacteria to adhere to and travel into the urinary tract, causing infections. Additionally, hormonal changes can alter the balance of beneficial bacteria that normally help prevent infections. The result? More frequent and stubborn UTIs—something many of us can relate to.
Research insights on menopausal UTIs
Studies confirm that declining estrogen levels in menopause increase the likelihood of urinary tract infections. According to research postmenopausal women are up to 2.5 to 3 times more likely to experience recurrent UTIs compared to premenopausal women. The loss of Lactobacillus—a type of “good” bacteria found in the vaginal microbiome—makes the urinary tract more vulnerable to infections by harmful bacteria, particularly Escherichia coli (E. coli).
Research indicates that up to 15% of women aged 60-65 experience three or more UTIs per year. This increased susceptibility is largely attributed to the physiological changes associated with menopause.
In addition, bladder function can be affected by menopause. Studies have found that 45-63% of postmenopausal women experience some form of urinary incontinence, which can contribute to incomplete bladder emptying and increased UTI risk. Together, these factors explain why UTIs become more frequent during this time of life.
UTIs from perimenopause to postmenopause
Perimenopause: Hormonal fluctuations begin, and some women may notice occasional vaginal dryness or irritation, which could already increase UTI risk. Perimenopausal women have a 1.5 times higher risk of UTIs compared to premenopausal women.
Menopause: Estrogen levels drop dramatically, leading to thinner, less elastic urinary tissues and changes in bladder control. If not managed early, UTIs can become a recurring issue.
Postmenopause: Without proactive steps, the body’s defenses remain compromised, and recurrent UTIs may continue to disrupt daily life. The prevalence of UTIs in postmenopausal women can be as high as 15-20%.
Practicing good hydration habits, pelvic floor exercises, and promoting healthy vaginal flora during perimenopause can help reduce future UTI risks. Studies have demonstrated that starting vaginal estrogen therapy during late perimenopause reduced the incidence of UTIs by 50% over a two-year period – something for discussion with your healthcare provider to learn more.
Effective UTI prevention tactics
There are several steps we can take to prevent UTIs:
Stay hydrated: Drinking water throughout the day helps flush out bacteria from the urinary tract. Studies have found that women who increased their daily water intake by 1.5 liters had a 50% lower rate of recurrent UTIs.
Consider vaginal estrogen: Topical estrogen creams or vaginal inserts can restore moisture and strengthen the tissue lining of the urethra and vagina, helping prevent UTIs. A meta-analysis in Obstetrics & Gynecology showed that vaginal estrogen reduced the risk of recurrent UTIs by 36-75%. Something to discuss further with your healthcare provider.
Probiotics for vaginal health: Probiotics that contain Lactobacillus can support a balanced vaginal microbiome, reducing the risk of infections. A randomized controlled trial found that daily probiotic use decreased the risk of UTIs by 50% in postmenopausal women.
Empty your bladder regularly: Try not to “hold it” for too long, as this can give bacteria more time to grow. Fully emptying the bladder is key. The American Urological Association recommends urinating every 3-4 hours during the day.
Wear breathable fabrics: Opt for cotton underwear and avoid tight pants to reduce moisture and bacteria growth in the genital area. Women who wear cotton underwear have a lower risk of UTIs compared to those who wear synthetic materials.
Wipe front to back: It sounds basic, but wiping front to back helps prevent bacteria from entering the urinary tract.
When to get professional help
While it’s normal to experience occasional UTIs, there are times when medical advice is necessary. Seek help if:
- UTIs are happening frequently (more than 3 in 6 months).
- Symptoms include fever, back pain, or nausea.
- There’s blood in your urine.
- Over-the-counter treatments aren’t working.
A healthcare provider may recommend tests, stronger antibiotics, or even hormone therapy to help manage the issue. The American College of Obstetricians and Gynecologists (ACOG) recommends seeking medical attention if UTI symptoms persist for more than 24-48 hours.
Experiencing recurring UTIs and don’t have time to get to the doctor? TreatMyUTI offers a convenient solution (within the United States). This online service provides quick and easy access to healthcare providers who can diagnose your UTI and prescribe treatment—all from the comfort of your home.
With TreatMyUTI, you can get:
- Same-day prescriptions sent directly to your local pharmacy.
- Convenient care from your home without waiting rooms or appointments.
- Expert help from qualified healthcare providers specializing in urinary health.
Getting fast relief is now as easy as filling out a short online form and connecting with a provider.
Check out TreatMyUTI to get your prescription in 1-2 hours.
Tool kit for UTI prevention
Here are some products that may help navigate UTIs:
Vaginal estrogen creams: Helps replenish estrogen locally without affecting the whole body. Studies have found that vaginal estrogen cream reduced the risk of recurrent UTIs by 60% in postmenopausal women.
Vaginal probiotic supplements support vaginal flora and urinary health. Brands like RepHresh Pro-B or Jarrow Formulas, which are specifically designed to support vaginal and urinary health. Look for products containing Lactobacillus rhamnosus and Lactobacillus reuteri, which have shown efficacy in preventing UTIs.
Cranberry supplements: While research is mixed, some women find them helpful in reducing UTI frequency. It’s suggested that cranberry products can reduce the risk of UTIs by about 26% in susceptible populations.
Bladder support teas: Herbal teas with ingredients like dandelion or nettle can promote urinary health. A review found that certain herbal teas may potentially help to flush out bacteria.